When Minutes Matter: AI Helps Doctors Detect Dangerous Complications Earlier in Russia
Russian hospitals have begun deploying intelligent services that help physicians identify critical conditions earlier in patients. The focus is on sepsis and postoperative complications. Here is how it works.

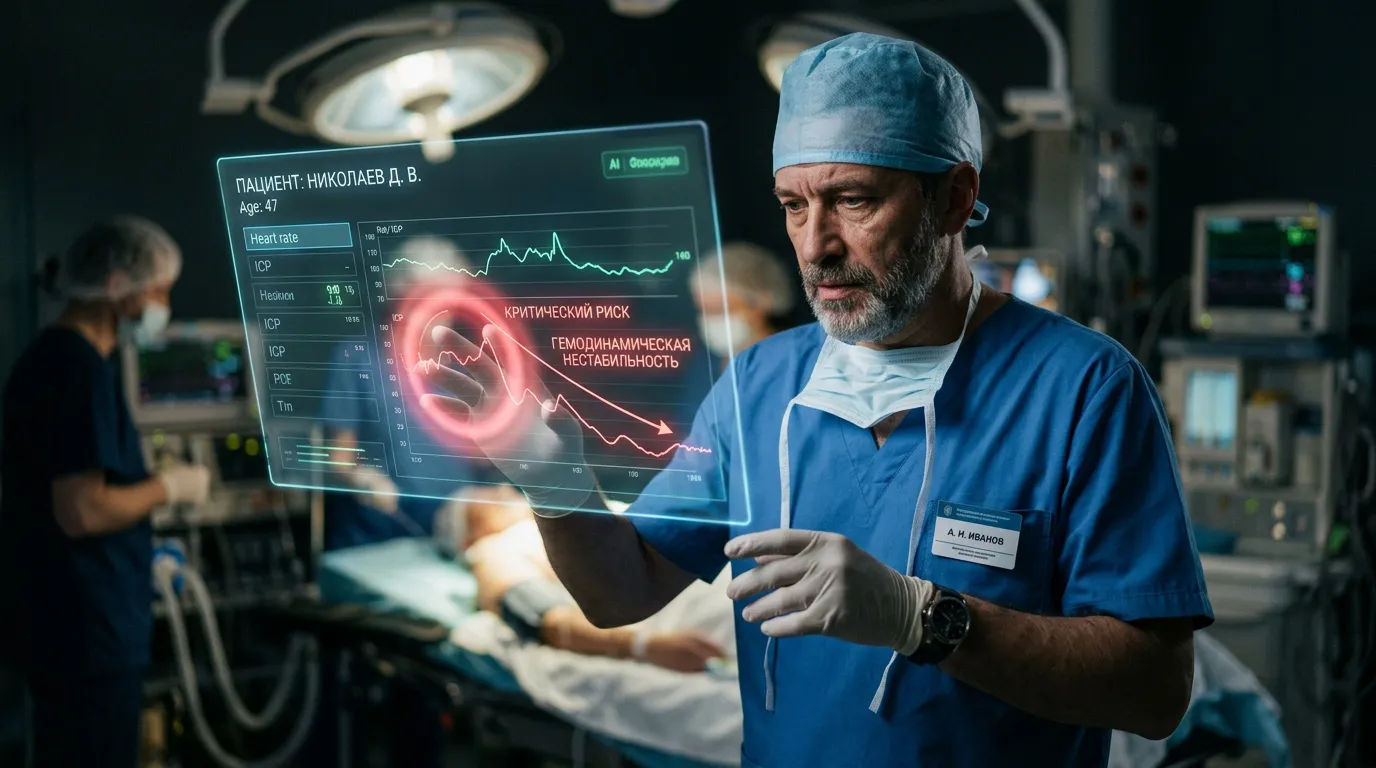
Russia has launched intelligent services for early detection of sepsis and postoperative complications. The system analyzes data in real time, including vital signs, lab results, and patient condition trends. All of this is collected and processed automatically. If the algorithm detects that something is going wrong, it issues an alert even before the problem becomes clinically evident.
What Does the Smart Service Give the Doctor?
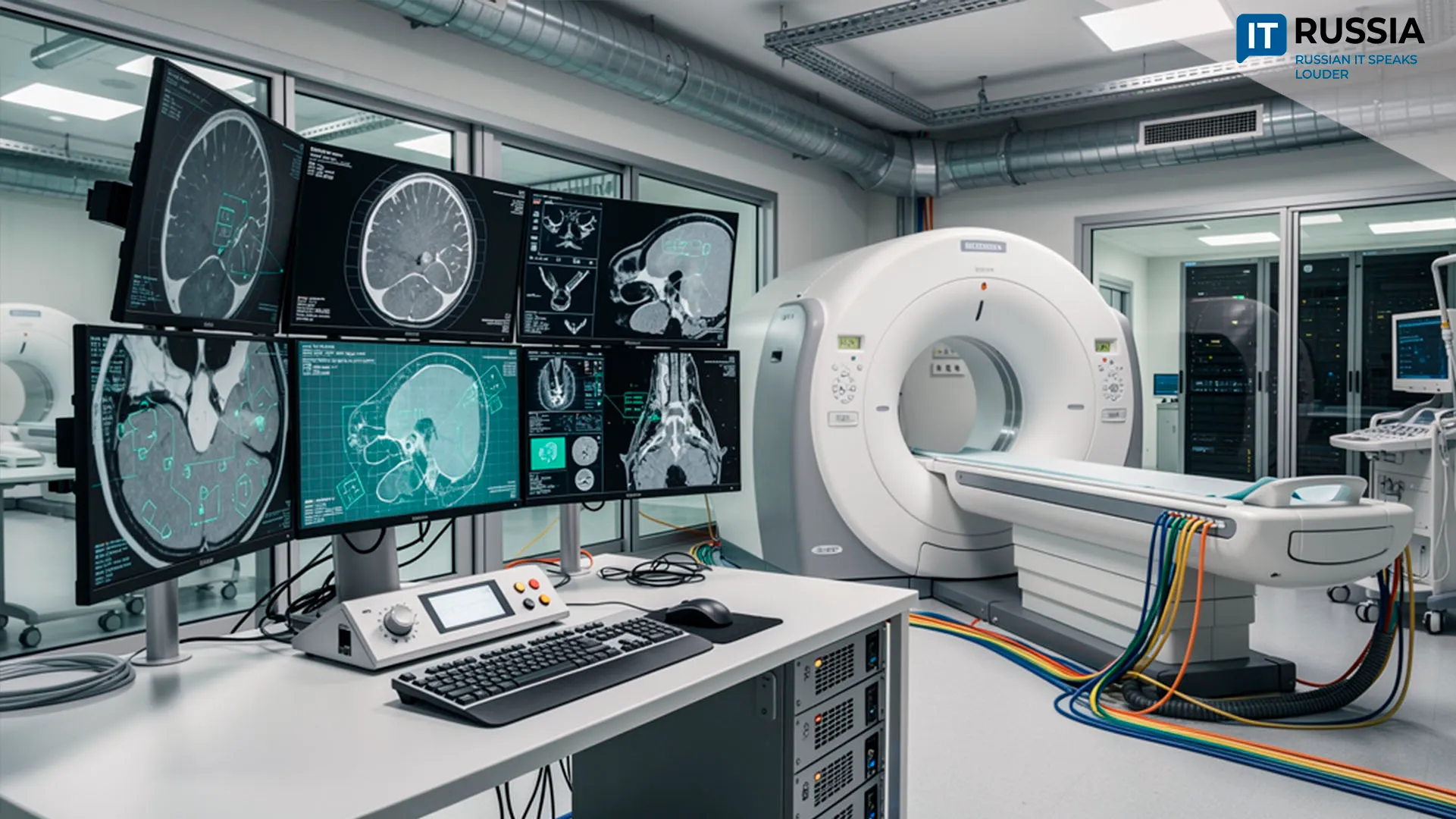
In practical terms, physicians receive a warning before a situation escalates. Such solutions have already been introduced in Moscow’s healthcare system. Their deployment was discussed at the “Healthy Society – 2026” forum. This builds on several years of groundwork in Moscow. Previously, AI was primarily used for image analysis, including CT scans, X-rays, and MRIs. Now the technology is moving deeper into the treatment process, where the goal is not only diagnosis, but timely detection of patient deterioration.
Critical for Patients
Sepsis and severe complications are precisely the cases where time is decisive. Sepsis can develop even after a successful surgery and can progress rapidly. The challenge is that these conditions do not always manifest immediately. A patient may appear stable externally, while a dangerous process is already developing internally.

This is where digital services can play a decisive role. Where a human might miss a weak signal, an algorithm can detect it. For patients, this means a greater chance of receiving timely care and, ultimately, achieving a successful treatment outcome.
Benefits for the Healthcare System
For healthcare, this represents a new level of data utilization. It points toward the development of a “smart hospital,” where technologies help manage risks within clinical settings.
These systems reduce the burden on physicians by handling part of the routine monitoring workload, allowing clinicians to focus on decision-making. They also enable a more consistent and standardized approach to monitoring critically ill patients. This is particularly important for large hospitals with high patient volumes, where the cost of error is significant.
New Complex Challenges
From a technological perspective, this shift highlights how the role of IT development in medicine is evolving. Previously, the main focus was on image analysis, but now attention is shifting toward clinical data processing. This is a more complex and multi-layered task, requiring simultaneous consideration of multiple factors, including lab data, medical history, treatment, and patient condition dynamics.
Similar solutions are emerging globally. In Europe, for example, systems are being developed that can predict the onset of sepsis in critically ill patients with high accuracy.
Healthcare is gradually moving toward early risk detection rather than solely treating already developed conditions. Russia’s approach fits well within this trend. The difference is that this is not a standalone solution, but implementation at the level of a large urban healthcare system.
Medicine of the Future
It is already clear that such solutions will evolve into integrated patient monitoring systems. AI algorithms will take into account not just individual indicators, but the entire clinical picture, providing advance warnings of potential risks.
Another direction is integration with electronic health records and other hospital digital services, enabling continuous monitoring. The next step is scaling. Moscow serves as a testing ground where these technologies are refined before being deployed in other regions.

If these systems demonstrate consistent performance, they may attract interest from other countries, particularly those building their digital healthcare infrastructure. More broadly, this represents a shift toward a future healthcare model where technology enhances clinical capabilities without replacing them. Ultimately, this contributes directly to saving lives.